Eye Love Optometry offers precise, individualized care for those suffering from or at risk of eye disease. We are dedicated to providing our community with the most advanced diagnostic technology, ensuring that we are best able to diagnose and manage a myriad of eye conditions and diseases.
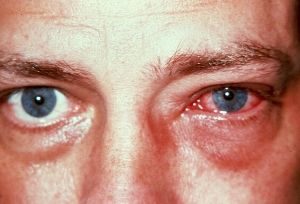
Conjunctivitis, commonly known as “pink eye,” occurs when the conjunctiva, the protective membrane covering the surface of the eye, becomes inflamed. This may be caused by bacterial, viral, and fungal infections as well as from a variety of different allergens and irritants, such as dust or smoke.
It is important to see your optometrist if you think you may have pink eye, so that the proper treatment can be prescribed. With the right care, most cases of conjunctivitis will clear up quickly.
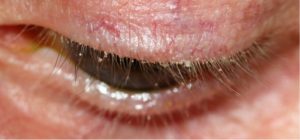
Blepharitis is characterized by inflammation in and around the eyelids and lashes. It is an extremely troublesome condition that is often difficult to manage without proper treatment.
Symptoms of blepharitis include red and swollen eyelids, itchy eyes, and flaky skin around the eyes. It can be caused by infection, an allergic reaction, mites, and poor eyelid hygiene. Fortunately, there are many treatments available for this condition. Your optometrist can help you manage blepharitis and find relief.
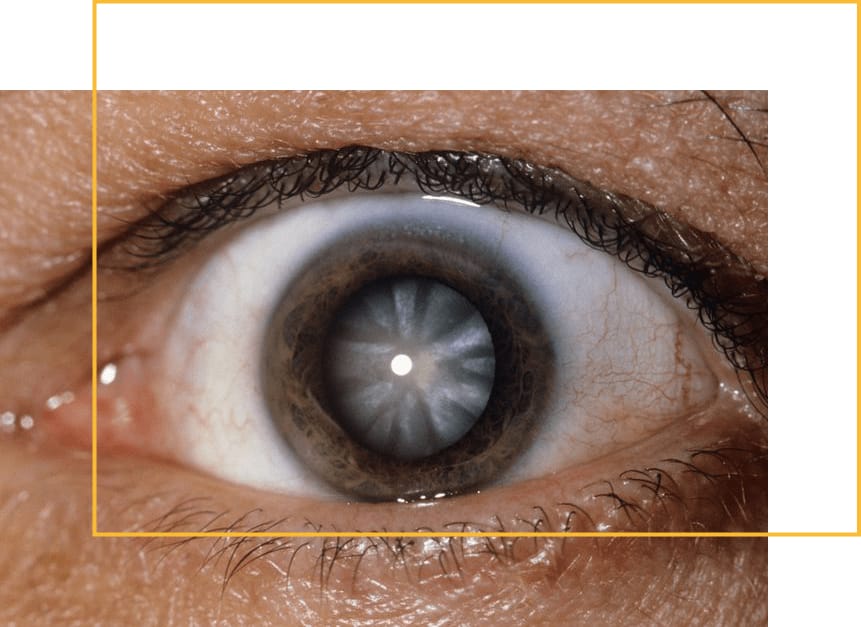 Cataracts are a very common condition in which the lens of the eye progressively clouds, becoming opaque. Cataracts appear gradually as we age, regardless of risk factors, but they may occur more rapidly or at a younger age depending on certain lifestyle factors, such as ultraviolet light exposure, smoking, and lack of antioxidants in the diet.
Cataracts are a very common condition in which the lens of the eye progressively clouds, becoming opaque. Cataracts appear gradually as we age, regardless of risk factors, but they may occur more rapidly or at a younger age depending on certain lifestyle factors, such as ultraviolet light exposure, smoking, and lack of antioxidants in the diet.
As cataracts develop, our team works with you to monitor and manage their progression. Should cataracts develop to the point of affecting your daily activities and lifestyle, cataract surgery will be recommended. We will co-manage your care with leading surgeons in the area.




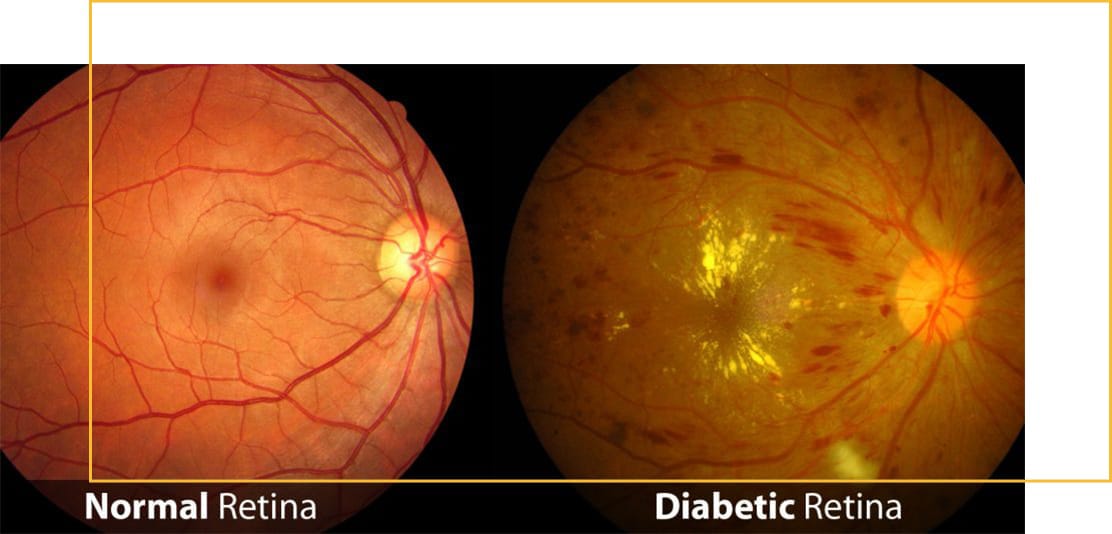 Individuals with uncontrolled diabetes may develop retinal blood vessels changes leading to bleeding, leakage, and strokes in areas lacking oxygen (retinopathy), as well as swelling in the area of the retina responsible for central vision (macular edema). They are also at a much higher risk of developing other eye diseases, such as dry eyes, cataracts, and, when more severe, glaucoma. Diabetic eye disease is a leading cause of blindness in individuals aged 15 to 64, so people who have diabetes should have their eyes examined at least annually.
Individuals with uncontrolled diabetes may develop retinal blood vessels changes leading to bleeding, leakage, and strokes in areas lacking oxygen (retinopathy), as well as swelling in the area of the retina responsible for central vision (macular edema). They are also at a much higher risk of developing other eye diseases, such as dry eyes, cataracts, and, when more severe, glaucoma. Diabetic eye disease is a leading cause of blindness in individuals aged 15 to 64, so people who have diabetes should have their eyes examined at least annually.
Read more about our Diabetic Eye Exams.




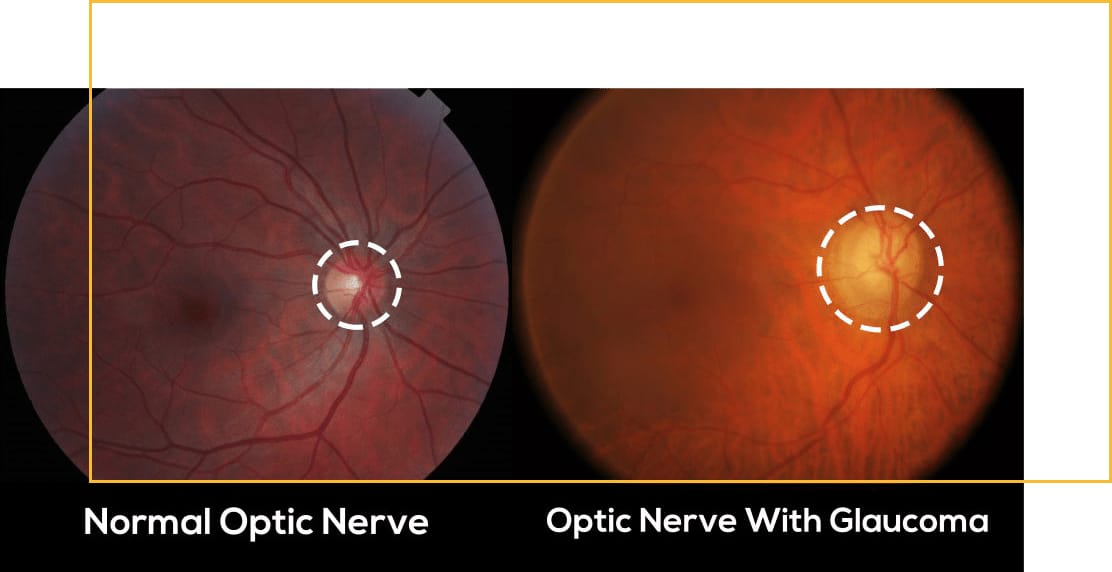 Glaucoma involves damage to the optic nerve, oftentimes but not always associated with high eye pressures. It is usually an insidious, slowly progressive disease with no initial symptoms, typically affecting peripheral vision first before central vision. When detected and treated early, the likelihood of significant and permanent visual impairment is reduced.
Glaucoma involves damage to the optic nerve, oftentimes but not always associated with high eye pressures. It is usually an insidious, slowly progressive disease with no initial symptoms, typically affecting peripheral vision first before central vision. When detected and treated early, the likelihood of significant and permanent visual impairment is reduced.
Over 3 million Americans suffer from glaucoma, and it is a leading cause of vision loss and blindness worldwide.




Age-related macular degeneration (AMD) is the leading cause of severe and permanent vision loss in individuals over the age of 60. It is defined by the deterioration of the macula, the part of your retina responsible for central vision.
AMD affects your ability to drive, read, recognize faces, and other important day-to-day functions. It often will not show symptoms until vision loss has already begun to occur. As such, it is extremely important to have your eyes examined regularly, so that this disease can be detected and managed as early as possible.
Read more about our Adult & Senior Eye Exams.




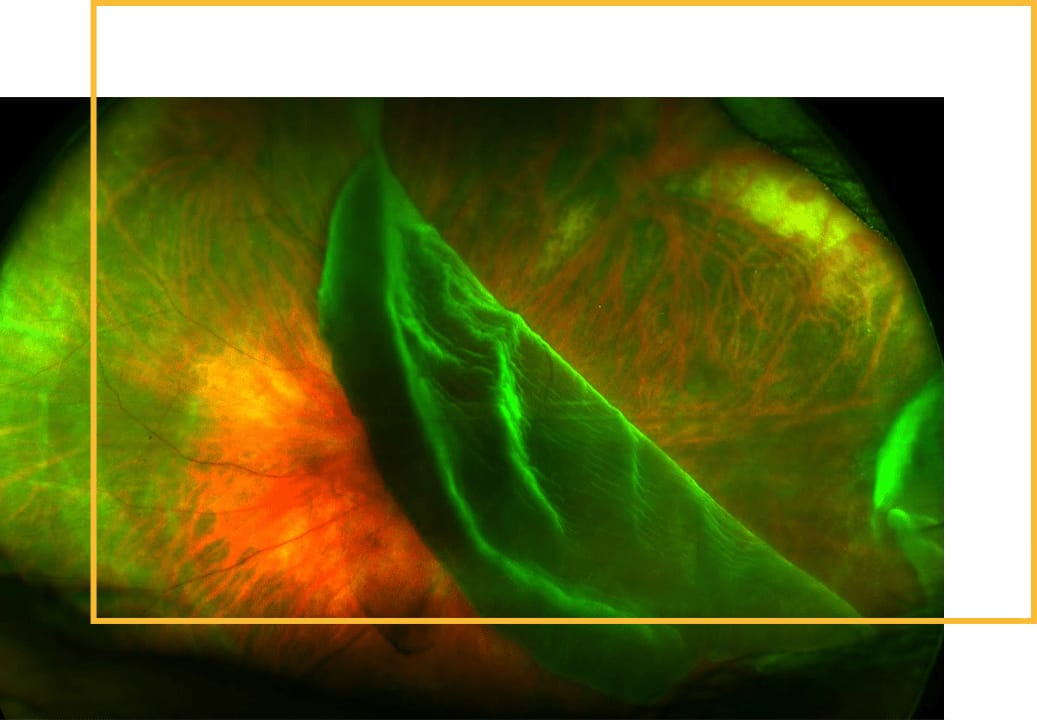 Retinal holes and tears occur when the gel-like substance inside your eye (vitreous) shrinks, tugs, and causes a break in the layer of sensory tissue lining the back of your eye (retina), which can be caused by injury to the eye. They are often accompanied by symptoms, such as floaters and flashes of light.
Retinal holes and tears occur when the gel-like substance inside your eye (vitreous) shrinks, tugs, and causes a break in the layer of sensory tissue lining the back of your eye (retina), which can be caused by injury to the eye. They are often accompanied by symptoms, such as floaters and flashes of light.
A retinal detachment is defined by the presence of fluid under the retina. This usually occurs when fluid passes through a retinal tear, causing the retina to lift away from the underlying tissue layers. Such breaks in the retina can be addressed by laser treatments, cryotherapy, and other surgical interventions.




Truly Innovative Technology
Eye Love Optometry offers our patients a wide array of advanced diagnostic technology, unmatched in their ability to detect the most subtle retinal changes. The tools we utilize ensure that we are always abreast of the ever-changing landscape of ophthalmic and optical science, allowing us to provide the most comprehensive care with the utmost precision and accuracy.
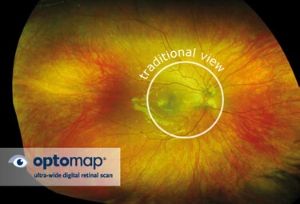
The Optos Daytona Plus generates an Optomap by using LASER-DRIVEN DIGITAL SCANS to create a 3-dimensional, ultra-widefield road map of your retina. Just because you see well does NOT necessarily mean that your eyes are healthy, and the Optomap is the BEST SCREENING DEVICE available to help detect the earliest changes caused by diseases, such as high blood pressure, diabetes, high cholesterol, glaucoma, macular degeneration, eye cancer, & retinal breaks BEFORE you notice any change in your central vision. It becomes a permanent part of your medical record, which can be compared to future scans to detect subtle, otherwise undetectable retinal health changes. Although not a substitute for getting your pupils dilated (associated with light sensitivity and inability to see up close), the Optomap is a good alternative by imaging 82% of the retina with a single capture, and 97% with four captures.
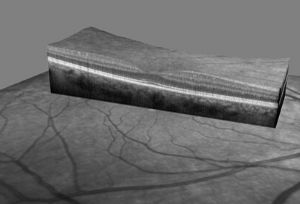
With an advanced retinal tracking system, the Carl Zeiss Meditec Cirrus HD-OCT provides the framework to precisely and comprehensively assess any retinal condition. 3-DIMENSIONAL DATA CUBES, exquisitely depicting each retinal layer, are registered with data from prior visits, allowing us to visualize the same retinal location, side-by-side, over time. A THICKNESS CHANGE MAP generated helps us to determine the next steps in treatment.
For glaucoma patients, in particular, no other device offers a more complete suite of INTEGRATED GLAUCOMA DIAGNOSTICS, which include retinal nerve fiber layer, optic nerve head, anterior chamber drainage angle, central corneal thickness, and ganglion cell analysis assessment. Along with Guided Progression Analysis™ (GPA), which provides a powerful tool for determining change in retinal nerve fiber layer and optic nerve head parameters, the SD-OCT sets the GOLD STANDARD IN THE STRUCTURAL ASSESSMENT OF GLAUCOMATOUS CHANGES.